Understanding the menstrual cycle: phases, hormones and visual insights
The menstrual cycle is a complex, recurring process that prepares the female body for potential pregnancy. It involves a series of hormonal changes that regulate the development and release of an egg, as well as the preparation of the uterine lining for implantation. A typical menstrual cycle lasts about 28 days, but it can vary between individuals, ranging from 21 to 35 days (NHS, 2024).
Phases of the menstrual cycle
The menstrual cycle is divided into four main phases:
Menstrual phase (days 1–5)
This phase begins on the first day of menstruation, where the uterine lining (endometrium) sheds, resulting in menstrual bleeding. This occurs due to a drop in progesterone and oestrogen levels, indicating that pregnancy has not occurred (Britannica, 2024).
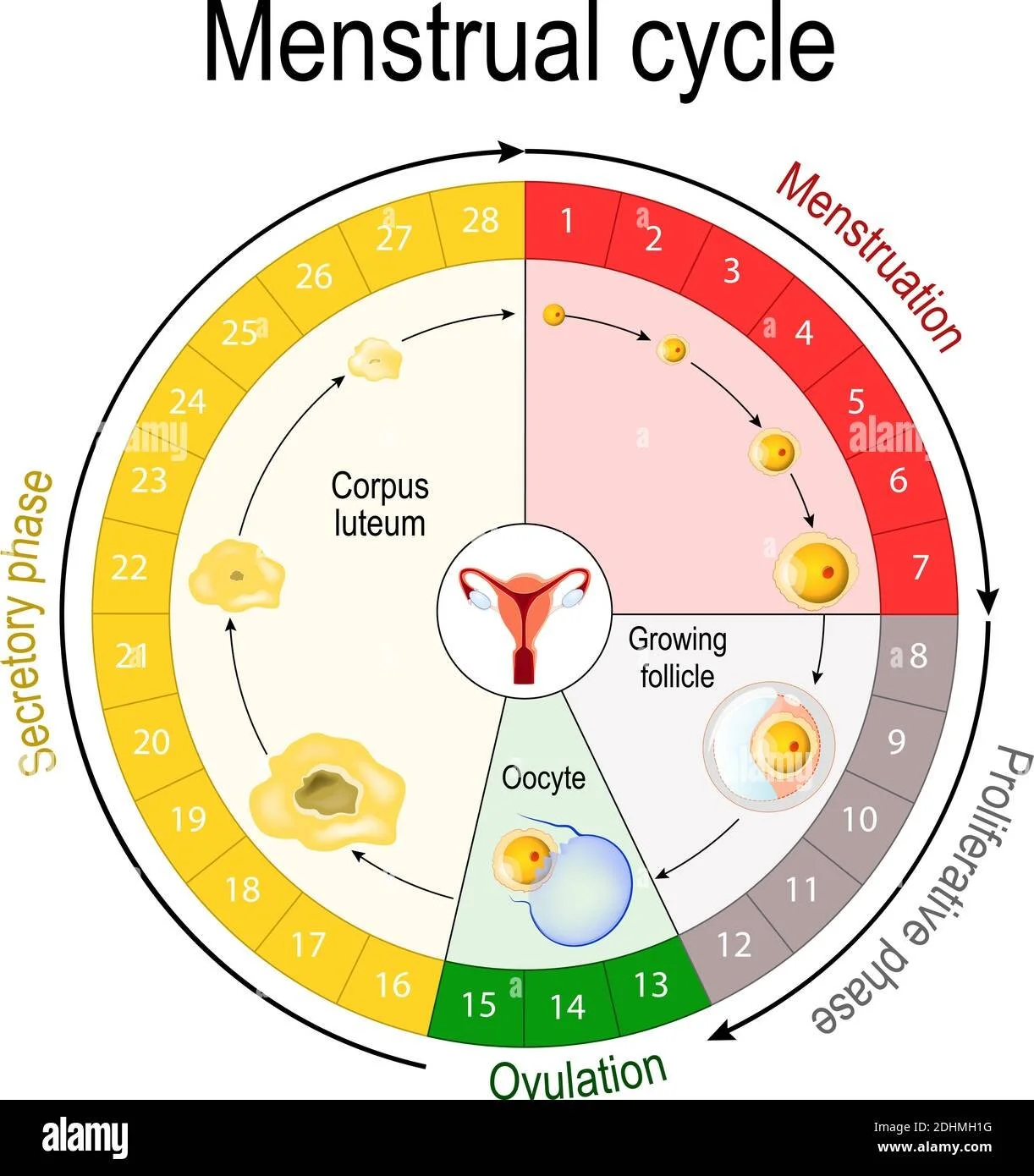
Figure 1: Menstrual phases
Follicular phase (days 1–13)
Overlapping with the menstrual phase, the follicular phase starts on day one and continues until ovulation. During this time, the pituitary gland releases follicle-stimulating hormone (FSH), stimulating the ovaries to produce follicles. Each follicle contains an immature egg, but typically only one reaches maturity. As the follicles develop, they secrete oestrogen, which helps rebuild the uterine lining (Britannica, 2024).
Ovulation (day 14)
Mid-cycle, a surge in luteinising hormone (LH) triggers the release of a mature egg from the dominant follicle in the ovary—a process known as ovulation. The egg then travels through the fallopian tube, where it may encounter sperm for fertilisation (Britannica, 2024).
Luteal phase (days 15–28)
Following ovulation, the ruptured follicle transforms into the corpus luteum, which secretes progesterone. Progesterone further thickens the uterine lining, creating a supportive environment for a potential embryo. If fertilisation does not occur, the corpus luteum degenerates, leading to a decline in progesterone and oestrogen levels, and the cycle restarts with menstruation (Britannica, 2024).
Key hormones involved
Follicle-stimulating hormone (FSH): Stimulates the growth of ovarian follicles in the follicular phase.
Luteinising hormone (LH): Triggers ovulation and the formation of the corpus luteum.
Oestrogen: Produced by developing follicles; it rebuilds and maintains the uterine lining and regulates FSH and LH levels.
Progesterone: Secreted by the corpus luteum; it stabilises the uterine lining for potential implantation.
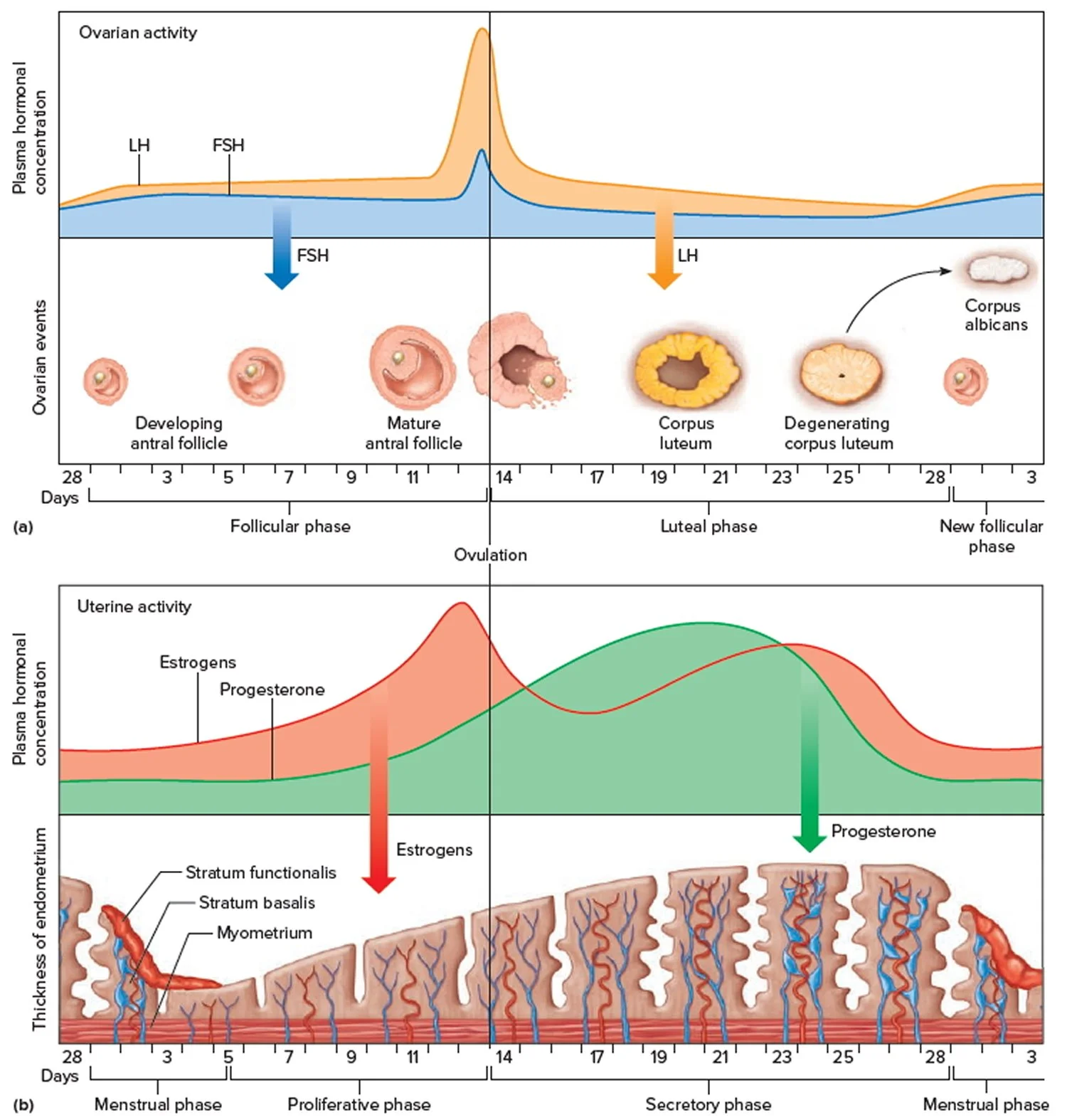
Figure 2: Ovarian activity during the menstrual cycle Source: https://healthjade.com/what-is-the-function-of-the-ovaries/
Visual representation of the menstrual cycle
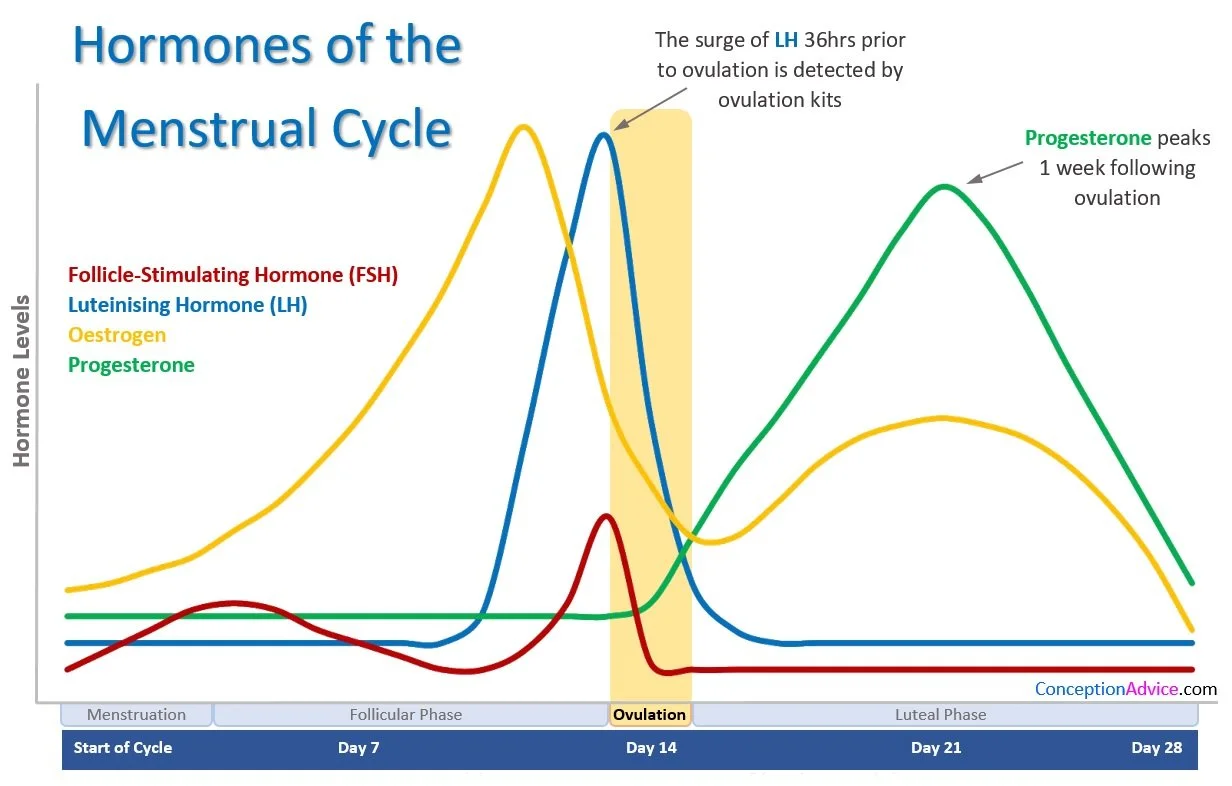
Understanding the hormonal fluctuations and physiological changes can be enhanced through visual aids. Figure 3 illustrates the phases of the menstrual cycle, corresponding hormonal levels and changes in the uterine lining.
Figure 3: hormones of the menstrual cycle Source: https://www.conceptionadvice.com/menstrual-cycle-calendar-phases/
Conclusion
The menstrual cycle is a finely tuned process orchestrated by hormonal interactions that prepare the female body for reproduction. Recognising the phases and hormonal dynamics can aid in understanding reproductive health and managing menstrual-related concerns.
References
NHS. (2024). Fertility in the Menstrual Cycle. Retrieved from https://www.nhs.uk/conditions/periods/fertility-in-the-menstrual-cycle
Britannica. (2024). Menstrual Cycle. Retrieved from https://www.britannica.com/science/menstrual-cycle
Conception Advice. (2024). Menstrual Cycle Calendar and Phases. Retrieved from https://www.conceptionadvice.com/menstrual-cycle-calendar-phases/